 Another post inspired by lectures in the Memorial Sloan Kettering Oncology Acupuncture course* What if the treatment that is supposed to save you causes so much suffering that you just want to quit? "Patients with cancer often fearfully anticipate the prospect of many potential negative consequences resulting from antineoplastic chemotherapy. At or near the top of their concerns is the common adverse effect (AE) of chemotherapy-induced nausea and vomiting (CINV). "When CINV goes untreated, it affects upwards of 60% to 80% of patients with cancer. CINV not only negatively impacts the quality of life (QOL) of the patient, but also the QOL of the patient’s family. Without prevention and control of CINV, patients may experience many undesirable events that can affect their QOL and/or treatment outcomes, including discontinuation of chemotherapy, which highlights the need for adequate prevention and control measures." (link) Management of nausea and vomiting in this population is sometimes a matter of life and death. Slightly less dire is the scenario in which it becomes "merely" an appallingly distressing symptom -- one so severe that physical symptoms can be triggered by association and appear in anticipation of the next scheduled administration of chemotherapy. Current anti-nausea guidelines include NK1 and 5-HK3 receptor antagonists, corticosteroids, and antipsychotic medication. The level of clinical research evidence for the efficacy of these drugs is high, and the benefits are considered to outweigh the harms. How does acupuncture compare to these top-line drugs? Can we compare them head-to-head, putting aside the common side effects of the pharmacological medications? The most recent overview of systematic reviews (from 2017), published in the Nature research journal Scientific Reports, concludes that "In the context of current best practice, acupuncture and related therapies may be considered as additional treatments to the guideline-recommended treatment with glucocorticoids, 5-HT3 antagonists and/or NK1R antagonists in patients with moderate or high risk of emesis." Diving into the studies comparing acupuncture to standard care summarized in that article, a 2006 Cochrane review concluded that acupuncture reduced incidence of vomiting, but not acute or delayed nausea severity, and added that "[this] review complements data on post‐operative nausea and vomiting suggesting a biologic effect of acupuncture‐point stimulation." It does not appear that there is evidence to support the acupuncture being superior to the standard regimen of receptor antagonists, steroids, and antipsychotics. This takes us back to the original question -- how effective is acupuncture? Although acupuncture is not as effective in controlling nausea and vomiting as the top-line pharmacological medications, it has been proven to be effective compared to placebo. It also has the singular advantage of producing no negative side-effects, unlike common anti-nausea drugs, which include Zofran (constipation, headaches), Emend (fatigue, hiccups), Decadron (insomnia, hyperglycemia), etcetera. In conclusion, for individuals who: 1) Do not tolerate standard anti-nausea medication well, 2) Tolerate medication but are getting minimal relief, or 3) Do not want to take additional medication... Acupuncture is a safe, effective, evidence-based option for symptom relief and improving qualify of life! *Oncology Acupuncture for Chemotherapy-Induced Nausea and Vomiting, with Gary Deng, MD, PhD and Matthew Weitzman, LAc
0 Comments
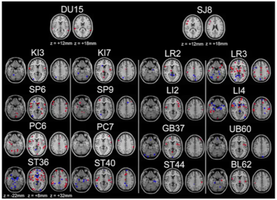 Image from Gary Deng, Medical Director of MSK Integrative Medicine Service Image from Gary Deng, Medical Director of MSK Integrative Medicine Service While listening to a lecture by Jun J. Mao of Memorial Sloan Kettering Cancer Center on the topic of acupuncture for cancer-related pain, I was struck by a comment about the areas of the brain that have been demonstrated to respond to acupuncture -- "[Acupuncture] not only stimulates […] somatosensory areas correlated with the needling area, but most importantly [also stimulates] the limbic system affecting cognition and emotion. As we know chronic pain is not just the physical experience of pain, but is also the psychological and cognitive experience of pain. [This is] probably why acupuncture can be a very effective tool in controlling both acute and chronic pain." This comment was in reference to a systematic review and meta-analysis of fMRI studies done by Claudia M. Witt's group, which concluded that "Brain response to acupuncture stimuli encompasses a broad network of regions consistent with not just somatosensory, but also affective and cognitive processing." Chronic pain -- where pain persists beyond the physical healing process -- has been described as a disorder of the central nervous system, leading to multiple network activation involving sensory, emotional, cognitive, and behavioral changes. As a clinician I see patients' quality of life improve in ways that go beyond just their reported reduction in pain. It is interesting to reflect on that in the context of the quote above, and the fMRI evidence of changes in sensory, affective, and cognitive areas of the brain. Pain is more than just a physical experience, and full recovery from chronic pain involves more than just a lower number on a 0-10 Likert scale!  An interview request for our local Crazy Wisdom Journal provided an opportunity for some reflection on these crazy times... What's the most difficult thing personally that you had to deal with during this time of stay-at-home orders and limited openings? How did you cope? Am I essential? Do I provide services that people rely on? Being hit with this professional question in the midst of an emergency led to a little bit of an existential crisis, which resolved only when my patients themselves expressed how important the treatments were to them. Besides that first scary week in March, where it seemed that the virus might be everywhere and anywhere, I feel fortunate overall to have experienced the pandemic primarily as a big pause, a big timeout — which brought with it an opportunity to reconsider where I wanted to put my energies. In my case that meant reorienting myself to be more “local.” More time with my family, more focus on my home and garden and the surrounding environment, and more focus on my local community and local issues. I’ve spent the last several years volunteering for state-level issues (which I have no regrets about), but I’m excited about “bringing things home,” so to speak, and keeping my attention here for the next decade or two! How have you had to pivot your business during this pandemic to continue taking care of clients? Acupuncturists have always been aware of the potential for infection, so that safety training is baked into our practice from the start. The big pivot was from blood-born pathogens to an air-born virus. That has required some practical changes in our practice and in the patients’ experience. Instead of just performing clean-needle technique to prevent cross-infection, we are now doing “the big four”: prescreening, masking, disinfecting, and filtering! My colleague Meagan Bretz and I now do all initial visits via telehealth, which has been surprisingly effective and welcomed, and we’ve built extra time into the schedule for cleaning the rooms between appointments. I wish we could still have patients come early and drink tea in the waiting room, but instead we ask them to call from their car, and then come in to get their temperature taken, after which they go directly to their treatment room. By the time they arrive at the clinic they will have already answered the Covid screening questionnaire, but the additional steps help protect the health of our staff and other patients from the possibility of any of us being asymptomatic carriers. Masks are required, of course, and new equipment filters the air during and between each patient visit. As long as all of these conditions are met, I find myself able to be fully present with patients without the distraction of fears about the virus, almost like it was in “The Before Times,” and I’m able to practice knowing that I’m protecting my patients, colleagues, and family. How can acupuncture help someone cope with the stress and/or fear of illness? Decision-fatigue is a real thing! Trying to assess risk and make decisions takes a toll on the mind and body, and many people feel like they are trying to do this every day. Yesterday I happened to be reading through a new meta-analysis of acupuncture during IVF, which concluded that beyond the positive effects on fertility, there was also a notable reduction in anxiety — equivalent to the positive results of doing group therapy. Results like that reinforce what many acupuncturists and patients have already observed, that regardless of the primary issue that is being addressed, the experience of getting regular acupuncture treatments is highly relaxing and de-stressing. We always take the time to talk with patients before doing a treatment. I consider that to be an essential diagnostic step, but I don’t doubt that it also helps with stress. Voicing one’s concerns in a therapeutic environment is often the first step towards letting go of any unnecessary concerns, and identifying the important ones. It’s in the acupuncture treatment itself where a lot of the magic happens, as parasympathetic activation allows “fight or flight” to give way to “rest and digest.” I choose certain acupuncture points, in particular those on the ears, specifically to elicit this relaxing effect. Modern research into the external innervation of the vagus nerve, which only occurs on the ear, has helped us flesh out the anatomical mechanism underlying our traditional approaches. The East Asian concepts of bringing Qi into empty channels, or of releasing it where it is stuck, predate our contemporary usage of the word “stress,” but the end result is the same — a move towards free thoughts and easy actions. What inspired you to practice acupuncture? I didn’t start out wanting to do acupuncture, I started out wanting to do qigong! It just so happened that I moved to China in 2001, however, which meant that no-one was willing to teach me qigong due to its associations with Falun Gong (this was just two years after the political crackdown on the group). Acupuncture and tuina and herbal medicine were the backup plan. I can’t complain though, as twenty years later I’ve realized that qigong is best learned at one’s own pace, and that (in both China and the US) it is easier to support a family as an acupuncturist! How do you unwind after a day at the office? I’m writing this during summer, so that’s an easy one... I’ve learned not to rush indoors after getting home from work, but rather to first take a walk around outside (no mask!) and get the colors and shapes and patterns of nature in my eyes and ears. The key is remembering to do it “this time, each time.” We are in the midst of a beautiful summer! Let’s take our time and enjoy it. https://crazywisdomjournal.squarespace.com/weekly-21 A little public service translation here, for anyone interested in the the text Fu Xing Jue Zang Fu Yong Yao Fa《輔行訣臟腑用藥法要》(Auxiliary Knacks of Essential Drug Usage for Viscera).
Ma Jixing first brought attention to this text, and in 1988 published the following story about its discovery: 关于《辅行诀脏腑用药法要》 Regarding the rediscovery of FXJ 十九世纪末,河北威县中医张偓南氏家传医学,所藏医书甚丰。敦煌卷子出土后,闻风前往,曾在驻洞道士手中重金购得医学卷子一轴。书名《辅行诀脏腑用药法要》。卷子首尾基本完整,其前尚绘有三皇、四神及二十八宿之图。张氏视为珍宝。殁后传于其孙中医张大昌(为靖)氏。大昌先生多取此书所载方论治病获有良效,并将此书教授弟子,且录有复本两种。 At the end of the 19th century, the family of Zhang Wonan of Wei County in Hebei practiced medicine, and kept an expansive collection of medical texts. After hearing rumors of the excavation of the Dunhuang scrolls, Zhang Wonan went in search of them, and purchased one scroll from the Daoist monk protecting the caves. The name of the text was FXJ. It was relatively intact and complete, and started with images of the three emperors, four spirits, and twenty-eight constellations. Zhang Wonan saw this as a treasure. After his death it was passed on to his grandson, the physician Zhang Dachang (style Weijing). Zhang Dachang frequently used the formulas and theory recorded in this text to treat illnesses with excellent results, and instructed his disciple with the text and created two copies. 1966年“文革”期间卷子不幸被毁。仅抄本幸免。1974年初张氏用“赤脚医生”之名将抄本寄送中医研究院。初未引起重视,后此件转交我手,经我反复考察验证抄件中保留与引用的古俗讳字、药名、药量、人名、方名、书名、篇名以及病症名称、方剂配伍特征、文章结构与风格等多方面内容,确定绝非今人仿造赝品。 Unfortunately the scroll was destroyed during the cultural revolution period in 1966, and only the hand-copies fortunately remain. In 1974 Zhang Dachang mailed a hand-copy to the Chinese Medicine Research Institute in his role as a barefoot doctor. At first it did not raise any interest, and later it came into my hands. I repeatedly researched and verified that the writing conventions, taboo terms, medicinal names and dosages, individual’s names, formula names, book names, chapter names, as well as disease names, formula composition characteristics, the text’s structure and style, all demonstrated that this could not be a contemporary forgery. 其成书下限绝不晚于宋初以前,因而由我写出了对该卷子年代的初步鉴定资料。为了进一步征求有关文史专家的意见,1975年我曾将此卷子释文及其有关情况,请教了社会科学院张政烺和李学勤两教授。经他们鉴定,在结论中也提到:“此书不是近代的伪作,但也不可能早到(南北朝)梁代的作品。作为一种古籍的传抄本,还是有保存的必要的。” The latest possible date of creation could not be later than prior to the beginning of the Song Dynasty, and for this reason (?) I have written up initial appraisal material. In order to solicit more opinions from other experts in the fields of literature and history, in 1975 I prepared an annotated copy of the text, with an explanation of its circumstances, and requested the guidance of professors Zhang Zhenglang and Li Xueqin of the Academy of Social Sciences. After their appraisal, in their conclusion they stated: “This book is not a modern forgery, nor can it be a product from as early as the (Northern and Southern Dynasties) Liang Dynasty. As an example of a hand-copy of an ancient text, it is necessary to preserve it.” 与此同时我院王雪苔同志也对此书寄予了很大重视。并专门就此事直接去威县张大昌先生处做了详细调查。并进一步获见保存与其弟子处的另一抄本。 At this time Comrade Wang Xuetai of my institute also expressed great interest in the text, and for this express purpose traveled directly to Zhang Dachang’s place in Wei County to perform an inspection. He was further able to obtain a separate hand-copy preserved at Zhang Dachang’s disciple’s place. 故本书此次的整理即特约请王雪苔院长据此两本互勘而厘定。 In the preparation of this book I specially engaged Director Wang to compare and collate these two copies. Dun Huang Gu Yi Ji Kao Shi 敦煌古醫籍考釋 (Commentary and Research on Ancient Medical Texts Excavated in Dunhuang, Ma Jixing 馬繼興, ed., Nanchang: Jiangxi Kexue Jishu Chubanshe, 1988, p. 4)  It nice to see one's work critiqued by a sincere reader; even nicer when the review is positive! Steve Clavey, editor of The Lantern, is clearly familiar with the original Chinese version of this book. His review of the recently published English version, the translation of which I contributed to, draws upon this familiarity to emphasize an important point: "...anyone who is drawn to take a deeper look at Chinese medicine theory should own and read this book. But it should not be read as a bible, or to “find out what is true” or to memorize." The author of this book, Liu Lihong, is a brilliant contemporary Chinese philosopher, writer, and commentator in the tradition of Lin Yutang and Chiang Yee (The Silent Traveller), to name two that might be familiar to an English-language audience. Although this book ostensibly focuses on the relatively specialized field of Chinese medicine, his observations and inquiries are broadly relevant to the larger fields of Chinese philosophy, religion, language, and society. "Opening Classical Chinese Medicine at random, I come across this phrase: 'Looking briefly at the simplified form of the character mai (脉), the original meaning of the character yong (永) was ‘long’. When this concept of ‘long’ is placed within the frame of reference of history, it might be taken to mean ‘eternal’. When placed in the context of the natural world, this idea naturally resonates with the image of a river, long and constantly flowing …' and so the passage continues, linking pulse to the flow of water and to the moon, and the link between the moon and water, with its tides and cycles, rise and fall. This is the type of thinking that can plumb deep and draw to the surface meaning unavailable to shallow dippers." I'm pleased that Liu Lihong's distinctive approach to mulling over challenging questions has come across in this English translation. One of the joys of translating this text was in appreciating this approach -- taking apart the questions, tracing characters and phrases back to their sources in classical texts, and then bringing it all together to expose new meanings and interpretations. I'll leave Steve with the last word: "This is a book to weigh and consider, and rather than take it as dogma we should be considering and attempting to verify its conclusions in our lives and practices. Of course, that takes thought, and everything around us these days encourages us to leave the thinking to someone else." Please read Steve Clavey's full review in The Lantern here: https://www.thelantern.com.au/wp-content/uploads/2020/04/review_CCM.pdf The book can be purchased by the US distributers here: http://cup.columbia.edu/book/classical-chinese-medicine/9789882370579 I've been spending so much of my volunteer time on acupuncture-related legislation recently that when I was contacted about writing something for our local Crazy Wisdom journal this topic naturally sprung to mind . . . Which state do you think was the first to legalize the practice of acupuncture? You are probably thinking California, right? Or maybe New York? Did any of you guess Nevada? This is an unedited case study from my forthcoming book on chronic inflammation and Chinese herbal remedies. This case study is a translation from the Chinese, and it details the recent treatment of a patient with chronic canker sores by my teacher Dr. Peng Jian, of Changsha, China. It is notable because of the successful use of warming herbs, in a condition where they are usually contradicted. This case study is posted as an example of the treatment of a chronic inflammatory condition with herbal medicine, and is not intended to provide diagnostic or treatment advice. Enjoy! Liu X, male, 33 years old, resident of Changsha
First Visit: October 6, 2012 For more than ten years this patient had recurrent ulcers erupting unceasingly on his tongue and throughout his mouth, which only healed up for four or five days in each month. Over the years he had seen various ENT specialists in Changsha, Wuhan, and Beijing without obtaining relief. I could also see from his medical history that he had visited many of the better-known Chinese medicine physicians in the area, and had been prescribed modifications of the formulas daochisan, xiehuangsan, and shengmaisan, as well as precious medicinals and patent formulas such as xiongdan, niuhuang, zhongtongan, zhenhuangpian, etc. At various points he had been instructed to eat simple and mild-tasting foods, and to scrupulously avoid spicy or stimulating dishes. Although he followed these recommendations to the letter, the sores would still erupt, and the pain and discomfort never ceased. With the exception of this issue he was generally healthy and active and his bowel movements were regular. Besides having urine that was more yellow than normal, he reported no other symptoms. His tongue was pale, and his pulse was small and wiry. I prescribed a modified ganluyin: shenghuangdi (dosages deleted) shuhuangdi maidong tiandong erhuanshihu zhike yinchenhao huangqin pipaye renzhongbai (seven doses) Second Visit: October 13 After finishing seven doses of the prescription the patient’s sores had not healed and were still painful, and the patient had a sense that they were actually getting worse. I looked carefully at his tongue and noted three or four small ulcers distributed over both sides of the tongue. His tongue was fat (swollen) and pale, with tooth marks and a thin white coating. His pulse was small and wiry. I changed the prescription to a modified mahuangfuzixixintang: mahuang (dosages deleted) fuzi xixin banxia fuling ganjiang (blast-fried) erhuanshihu renzhongbai (seven doses) Third Visit: October 18 The patient had come early as he was about to leave on a business trip, and at the time of the visit he had not yet finished all seven doses of the prescription. He told me that by the time he had finished the second dose the pain had already gone, and by the fifth dose, which he had just taken, the ulcers had already healed. I observed that his tongue was much thinner (less swollen) than before, and it was still pale with a thin white coating. His pulse was thin and wiry. The patient also mentioned that every since he started getting oral ulcers he had also developed small lumps on his scalp, which were reddish and sensitive to pressure. This was in spite of having taken so many cold and cooling herbal prescriptions in the past. I re-prescribed seven doses of the decoction, and additionally prescribed the same formula in pill form for him to take on his trip: Pill prescription: mahuang (dosages deleted) fuzi xixin banxia fuling ganjiang erhuanshihu renzhongbai lurong wubeizi (the pill prescription was to be taken twice a day, 6g each time) Fourth Visit: November 22 The previous prescription had lasted about a month, and the patient came back in as he was running low. He said that in the last month he had not had a single ulcer appear, and in addition the lumps on his scalp had gotten much smaller. There was no need to change an effective formula like this, so I prescribed another month’s worth of pills to consolidate the treatment. Fifth Visit: March 11, 2013 After finishing the previous prescription the patient had not had any more oral ulcers, and the lumps on his scalp had disappeared. I observed that his tongue was still pale and had tooth marks. I added 30 grams of xianlingpi to the formula, and re-prescribed another month’s worth of pills. Lessons learned from this case Treatment: Generally speaking, oral ulcers are usually associated with a pattern of yin deficiency with damp heat. It is extremely rare to see them occur in a pattern of yang deficiency with cold damp. This was one of those rare cases. In the initial visit, although I noted that the patient’s tongue was pale with a thin white coat (in contrast to the usual red tongue with yellow coating of most oral ulcer sufferers), I still did not feel confident about using warm medicinals. It was quite possible that these signs of cold resulted from taking so many cold and cooling medicinals, rather than being a true sign of internal cold, so I was concerned about the possibility of adding fuel to a fire. The initial use of ganluyin was a way of testing the waters, and when it became obvious in the second visit that not only had the patient not improved, but even seemed to be getting worse, and now had a fat (swollen) tongue, I felt more confident about turning to warming methods, and prescribed mahuangfuzixixintang to warm the channels and disperse cold. Added to the formula were banxia to transform phlegm, fuling to leach out dampness, and ganjiang to warm the center. I was still concerned that this sudden change to warm herbs might cause lurking fire to float upwards, so I also added erhuanshihu to nourish stomach yin, and renzhongbai to clear deficiency fire from the middle burner. This approach turned out to be the right one. One of the factors that prompted me to re-write the formula from scratch was an offhand comment by the patient: “As soon as I see my tongue getting fat, and as soon as those tooth marks appear, I know things are going to get worse.” As the old saying goes, “Patients are our teachers”! If he hadn’t mentioned this information I might not have had the temerity to use such warm and hot medicinals! Book Review in JCM: "The Classic of Supporting Life with Acupuncture and Moxibustion Vol. I-III"10/22/2014  This is a book I've enjoyed for many years - I'm excited to see it come out in English! The Classic of Supporting Life with Acupuncture and Moxibustion Vol. I-III Lorraine Wilcox (Editor) Yue Lu (Translator) Reviewed by Henry Buchtel Wang Zhizhong was a man full of contradictions. On the outside a moderately successful teacher of Confucian learning, in his later years he gained renown instead for his private study and practice of the art of medicine. His text《針灸資生經》Zhenjiu Zisheng Jing contains the results of his studies – page after page devoted to resolving age-old discrepancies in the recorded locations of traditional acupoints, and passage after passage recording his own clinical experience in locating the most effective acupoints for specific patients at the time he treated them. Why then, when his own experiences with patients showed that the exact location of an acupoint could be found through palpation, did he still devote so much effort to recording and standardising the location of named acupoints? This is the question that I brought to this new and exceptionally accessible English translation of the Zhenjiu Zisheng Jing: The Classic of Supporting Life with Acupuncture and Moxibustion (Volumes I to III). In this day and age, where textbooks feature descriptions of the locations and routes of acupoints and channels as if they were incontrovertible fact, it is easy to assume that these areas and connections have always been agreed upon, and that there is no disagreement among the various authoritative texts. This was by no means assumed to be true by Wang Zhizhong, as can be seen in Volume I. Here he lays out the result of his efforts to reconcile the different standards for acupoint location and cun measurement methods, and sets out a single standard for both. His influence on later generations can be seen when it comes to the location of abdominal points, where his chosen standard of 1.5 cun (measured using the distance between the creases of the middle finger as one cun) between the Kidney, Stomach, and Liver channels on the abdomen was used by texts for the next half-millennium, including such classics as the Zhenjiu Dacheng, (Great Compendium of Acupuncture and Moxibustion). However, Wang Zhizhong made no effort to conceal evidence of any discrepancies between his sources, and in fact took great care to leave behind a record of his thought process and the names of the texts to which he referred. This takes us to Volume II, where in this careful translation written in natural and idiomatic English, we find an unusual treat – more than a dozen of Wang Zhizhong’s personal essays on matters relating to moxibustion, acupuncture, herbs and the art of healing. For example: ‘Qian Jin Yao Fang says: There are old and young people, with tall and short bodies, fat and thin skin. So we need to consider this thoroughly and discuss it, and be precise when locating points. [Points are located] in the muscles, in the cleft of the joints, or in depressions. Patients feel happy when we press these points. If we locate the points carefully, peacefully, and serenely, we can find them [accurately]., (2.08 Locating points) Such essays are a rarity among medical classics, which tend to be written in more of a distant and authoritative voice. However, as smooth and easy to read as this English translation is, one must still remember that Chinese texts of that time were not meant to be quickly devoured like the latest bestseller in the airport bookstore. As Wang writes, this material is to be ‘… considered thoroughly and discussed.’ These passages lend themselves to being mulled over, deliberated upon and perhaps committed to memory in the same way one might appreciate poetry. In a text like this that has been passed down for nearly a thousand years, it is rare for the complete text to have found its way to us unharmed. Even though I accept this, I still feel that it is a terrible loss to us that the last three of Wang’s personal essays did not survive. One of the three, titled ‘Zhenjiu Shou Bing Chu’ (‘Areas affected by disease in acupuncture and moxibustion’) might have helped us address the seeming contradiction that runs throughout his writing – the fact that Wang both palpated for areas of soreness to determine where to needle, and at the same time obviously placed great importance on determining the standard body-cun location of acupoints. In Volume III (as well as the forthcoming Volumes IV-VI) we find another unique aspect of the book: a listing of acupoints by disease with personal commentary. The phrase ‘area affected by disease’, or variations such as ‘[an area that] aches when pressed’, appear in Wang’s clinical commentary several times: ‘We should apply this moxibustion on the bony prominence that aches when pressed’ (Chapter 3.29, Bloody stool), ‘I pressed her Da Chang Shu and she felt sharp pain’ (3.33, Intestinal pain). The use of palpation to precisely locate effective acupoints, or to help determine whether or not to use a documented acupoint, is one of a great many traditional techniques that did not make their way into modern TCM textbooks in China or the West, a situation which has affected the way acupuncture and moxibustion is practised today. The situation in modern China was described by contemporary Chinese medical scholar Wei Jia (魏 稼) as follows: ‘For a long time we have emphasized the clinical application of static points [i.e. acupoints with names and fixed locations], while deep and broad exploration of dynamic points [i.e. acupoints that have no fixed name, location, or number and are often in a hidden or mobile state, requiring special diagnostic techniques to identify] has not elicited enough attention. [Changing this] will improve clinical results, and help to develop or even reconstruct acupuncture theory.’ ('动穴疗效钩玄'魏 稼 中医药通报 2008年 第7卷 第1期). It is exciting to think of the role that the publication of this translation might play in the continuing emergence of this hidden side of the medicine, and the influence it might have on future editions of college textbooks. I do not feel that in my reading of this text I was able to reconcile the deeper conceptual contradiction between the apparent existence of both static and dynamic points – one existing irrespective of individual or disease, and the other identifiable only in the moment. However, we can find a hint of justification for the efforts Wang took in standardising and recording acupoint locations in heartfelt quotes such as ‘If [he] had burned three or five hundred cones of moxibustion [as recorded in Tong Ren Shu Xue Zhen Jiu Tu Jing], the patient might have lived a long time, too.’ (p.76); or ‘Note that Su Wen – Ci Jin says: The patient will become limp if the patella is punctured and fluid comes out. Du Bi (ST 35) is located below the patella, on the shin bone. The acupuncturist must not disparage this.’ (p.134); and ‘I have saved more than a hundred people already’ (p.271). Lines such as these make it quite clear that Wang Zhizhong recognised the importance of transmitting and passing on the clinical pearls of his predecessors. One might say that Wang accepted that the process of naming and recording the location of acupoints, using the fairly consistent and accurate body-cun method, was the best way possible to pass on knowledge in a textual form – and this was valuable enough in and of itself to justify his efforts. This English translation, authored by Yue Lu and edited by Lorraine Wilcox, is published complete with the original Chinese, acupoint illustrations and a detailed table of contents and indices. Nearly one millennium after it was first published, in this text we are given access to a lifetime of scholarly and clinical experience in moxibustion, acupuncture and herbs. Henry Buchtel Published in The Journal of Chinese Medicine, issue no. 106 http://www.jcm.co.uk/product/catalog/product/view/13108/the-classic-of-supporting-life-with-acupuncture-and-moxibustion-vol-i-iii/  《秋天是某种思想陪着我》刘剑桦著 《秋天是某种思想陪着我》刘剑桦著 At The Scene In the middle of the street Lies a pile of broken glass There is no need to guess What just occurred This time, someone finished their drink And smashed the empty bottle on the ground A car, driving by The glass gives off a shimmer Of sound, delighting the ears 事故现场 马路中间 撒着一堆玻璃渣 不用猜测也知道 刚才发生了什么事 这时,有人喝完酒 将空瓶砸碎在地 一辆汽车驶过 玻璃渣,发出一片 悦耳的响声 From the collection Qiutian Shi Mozhong Sixiang Peizhe Wo, by Liu Jianhua, published in Chinese by Zhuhai Publishing Co., 2012. Translated here by Henry Buchtel, with help from Brodie Burris I'm reminded of the passage in 《養生論》where it talks about the power of emotions, in particular this line:“夜分而坐,則低迷思寐;內懷段憂,則達旦不瞑。” (loose translation: if one stays up late to work, he will feel quite sleepy; but if one's breast is full of worries, his eyes will be open all night)
In my case what it takes is a stimulating lecture and good conversation! |
AuthorPractitioner, Translator, Teacher Archives
March 2021
Categories |
 RSS Feed
RSS Feed